Article
The leader’s triangle
By Amy Edmondson | February 21, 2017

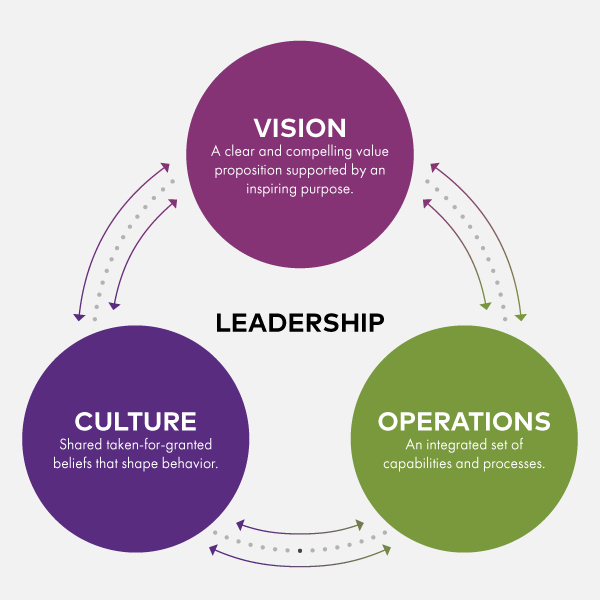
Alignment of those elements matters as much as the nature of the elements themselves. That’s because, taken together, these three levers constitute a powerful simplifying tool to help leaders assess their organization’s current state and consider what changes may be needed to sustain its success into the future.
From small clinics to major hospital and health systems, the Vision, Operations, and Culture framework is a model that should occupy a great deal of leadership attention.
Vision

Vision refers to clarity about where the organization is strategically headed and what value it seeks to add in its community or market. One of the most important decisions leaders must make in formulating a vision relates to the performance dimensions upon which the organization must excel to fulfill its promise to its customers, clients or communities.
Put another way: What dimensions of performance are most important to those whom the leaders seek to serve? Equally important, and far more difficult for most leaders, is answering the related question of what performance dimensions will not be prioritized. To illustrate this kind of clarity about performance dimensions, consider Southwest Airlines.
Founded on a value proposition of inexpensive, reliable, on-time, air travel, Southwest built a powerful enterprise around delivering on that promise. To succeed, Herb Kelleher, its founder and longtime chief executive officer, believed the airline must offer the lowest fares in the industry, and it must outperform the industry average in on-time performance. What it would not do is provide frills of any kind — no first class, no hot meals, no baggage transfer between airlines, and more.
Crystal clear about the value proposition, Kelleher was armed to resist the inevitable pull to offer frills that customers would seem to desire. This clarity about which performance dimensions matter is an organization's strategic value proposition, which requires making deliberate strategic decisions about how to compete effectively in a particular market.
The set of decisions the strategic value proposition represents falls within the umbrella category of “vision," because those decisions present a picture of who an organization is and what it uniquely wants to offer to the world. Note that a strategic value proposition is not in any way limited to the low end of the market. Leaders at Ritz Carlton are equally clear about which performance dimensions matter most to their success: impeccable staff service and exquisite facilities, for example. They are also clear about which performance dimensions they don't intend to optimize: price, for example.
Operations

Operations refers to an integrated set of capabilities and processes through which value is delivered. Note that operations exist as a result of leadership decisions — everything from whom to hire to what equipment to buy to what standard operating procedures to design.
Through these decisions, organizational capabilities are created.
For example, the single most critical capability Southwest Airlines needed, in order to deliver on its value proposition of low fares and on-time arrivals, was gate turnaround time. Each time a flight landed at an airport, staff would have to quickly turn around the plane to efficiently deliver a new set of passengers to a new location. Although at first glance it would seem Southwest eschewed meals to save money, these savings paled in comparison to those achieved by using the extraordinarily expensive equipment (the airplanes) more efficiently than any other airline (by keeping them flying rather than on the ground).
Thus, the real cost savings that accrued from not serving meals came from not waiting for catering at the gate — and thereby not risking that any non-core element of the strategic value proposition would interrupt and inhibit delivery on the firm's promise to customers.
To minimize gate turnaround time, Southwest employees are hired for teamwork and trained to do everything they can to work together seamlessly, across roles, to turn flights around quickly. In short, Kelleher knew that fulfilling the company's vision (inexpensive, reliable, on-time, air travel) depended entirely on the company's ability to build a particular set of operational capabilities — one that was fully aligned with that vision.
Similarly, Ritz Carlton selects and trains employees to deliver impeccable service when they come in contact with customers, and selects and decorates facilities to embody a particular impression and experience. It also developed standard processes to shape a consistent level of service, and empowers front-line staff to authorize unusually large expenditures to solve rare customer problems.
Culture

The subtlest of the three leadership tasks is building a culture that's magnificently aligned with the organization's vision and operations. An organization's culture consists of taken-for-granted assumptions about what matters, what's appropriate, how one should behave.
Leaders of the best organizations in every industry build their company culture on purpose — to dramatically increase the chances of reliably delivering on the organization's strategic value proposition. Culture tells employees how to behave in the absence of a formal rule (and in the absence of oversight). It's like a 24-hour a day training program — good news if leaders build a healthy culture — because it's working for organizations, day in and day out, for free, to help employees do the right things that matter for the value proposition.
And of course, if the culture is at cross-purposes with the vision or operations, this comes as bad news. At Southwest, Kelleher and his colleagues built a culture of teamwork, friendliness, humor, and fun that was superbly well-aligned with the company's vision and operations. To keep that culture alive, Southwest's hiring practices (an aspect of operations) are well designed to select people who will fit in well with the culture — people who have a sense of humor, are interested in other people, and are able to exhibit empathy and helpfulness when interacting with customers, particularly when facing the periodic frustrations that invariably arise with weather delays and other air travel issues.
Southwest does this through team-based interviews, even including its most loyal frequent flyers in the interview process. These customers love the airline so much, they're willing to give up some of their free time to help it hire new employees.
Ritz Carlton goes to extraordinary lengths to acculturate new hires, training everyone in its unique service culture of “ladies and gentlemen serving ladies and gentlemen." This mindset, and these skills, are well-aligned with the company's operational systems that hire and train stringently, and empower (within well-specified guidelines) front-line staff to deliver on the company's clear value proposition.
Leaders build an organization's culture in three ways:
- Often most important, their own behavior is a model that signals to others what matters, what's valued, and what to emulate, consciously and not. For instance, when leaders are compassionate, or curious, or celebrate well-intentioned risks that failed to produce hoped-for outcomes, their behaviors let others know which attitudes and behaviors are valued in the organization. Kelleher, for example, famous for his infectious sense of humor, would dress up in outlandish costumes for Halloween, encouraging others to express themselves in unique ways and to have fun at work. Southwest's culture of fun is a trademark element of the service — not intended to appeal to everyone, but rather to reinforce the core service model, helping customers cope with the frustrations of air travel, taking them all in stride. The culture also helps employees avoid blaming each other when things go wrong.
- Leaders coach and give feedback, continually sending verbal messages that shape and reinforce the culture.
- Finally, operational decisions related to hiring and training practices are a crucial force in creating a desired culture by design.
Using the Leadership Triangle in Health Care
Too often, leaders in health care delivery have not taken the time to articulate a clear and compelling vision or value proposition for their organizations. To do this well, it's important to bring people together from different parts of the organization, so as to consider multiple perspectives and build buy-in. The essential task is to figure out what performance dimensions must be prioritized. For instance, maybe the priority is patient satisfaction, with appointment wait times or digital communication as the key capability. Maybe clinical quality is more important, with success measured through high immunization rates or other aspects of population health.
Depending on the competitive landscape an organization confronts, different dimensions of performance may need to be prioritized to attract and serve patients. An FQHC may choose to prioritize access for patients over facility décor. What is most important is building a shared understanding of, and commitment to, a few selected indices of excellence (which quality metrics, which systems will be used to measure?).
Leaders must ask themselves and their colleagues the following question: “On what dimensions must we excel to earn the right to sustain our organization in its market/community for years to come?" And, correspondingly, what would be nice to have but may be less essential to our strategic value proposition (Ritz Carlton-level facilities, for instance)?
Having wrestled with these questions, the leader's second task is to assess the organization's operations by asking: What capabilities and processes must we have to excel in the ways we believe are crucial to our success? Finally, health care leaders must embrace their roles as stewards of the organization's culture. They should ask themselves: What must I do, how must I be, to set the right tone for the organization? What messages must I continually reinforce, and what systems must we design to hire and train people who can deliver on our vision? Each of these leadership activities is vital to the organization's success — but when aligned, added value is created through synergy.
The most successful and enduring organizations in every industry have found ways to leverage the synergy of alignment, but it doesn't happen by accident. It requires leadership. While each of the above categories encompasses crucial decisions and actions that affect organizational success, the true power of this model comes from ensuring alignment among them.
Amy Edmondson is the Novartis professor of leadership and management at Harvard Business School. Image credit: Michael Brook.





